PRODUITS
Masimo Patient SafetyNet™*
Système complémentaire de surveillance des patients et de notification des cliniciens
Le Patient SafetyNet est un système complémentaire de surveillance des patients et de notification des cliniciens qui affiche des données, en temps quasi-réel, de n’importe quel appareil Masimo ou tiers connecté, sur une station centrale, permettant l’envoi des alarmes et des alertes depuis les appareils de chevet directement aux cliniciens.
* La marque commerciale PATIENT SAFETYNET est utilisée sous licence du consortium universitaire des systèmes de santé (University HealthSystem Consortium).
Continuous Supplemental Monitoring
Customizable Central View Station
Patient SafetyNet allows clinicians to monitor up to 500 patients from a central view station.
The configurable display allows clinicians to view the status of up to 40 patients at a glance, as well as investigate alarms and dive deeper into trend data.
Remote Clinician Notification
Patient SafetyNet sends notifications to the assigned clinician via the Masimo Replica® mobile app.
When alarms are not addressed in a timely fashion, automated alarm escalation can help clinicians avoid potentially adverse patient events.

All alarms are set at the point-of-care device.

Patient SafetyNet provides a supplemental alarm notification system, making device information available outside the patient's room.

Escalating alerts and patient data are visible to clinicians on their mobile devices.
Case Study: Reduction in Mortality and Improved CPR Outcomes
In a before-and-after study conducted in a 1,200 inpatient bed facility, after the implementation of Masimo RD SET®, Patient SafetyNet, Replica, and a modified early warning score, researchers observed a reduction in all-cause mortality and improved resuscitative outcomes. In the post-deployment time period, patients connected to Patient SafetyNet were associated with:1
 27%
27%
better odds of survival1
 41%
41%
lower odds of suffering cardiopulmonary arrest1
 1.55X
1.55X
as likely to survive cardiopulmonary arrest1
 0.4 days
0.4 days
average reduction in length of stay1
Simplifying Workflows with ADT and EMR Integration
Patient SafetyNet and Root interface with hospital HL7 Admit Discharge Transfer (ADT) systems, allowing clinicians to associate patients with their data at the bedside through a drop-down list or barcode scanning.
Automatic Data Transfer
Automatic data transfer from medical devices to the electronic medical record (EMR) may improve productivity and reduce the likelihood of transcription errors.2
Automated Transmission and Recording
Patient SafetyNet automates the transmission and recording of key data from connected Masimo and third-party devices to the EMR, helping clinicians spend less time recording information and more time caring for patients.
Root + Third-party Standalone Devices
Root’s built-in Iris® ports act as a connectivity hub for third-party standalone devices.

Patient SafetyNet
Patient SafetyNet converts all Masimo and third-party bedside device data into HL7.

EMR
Patient SafetyNet automates data transfer from multiple devices to the EMR.
Scalability Matters
With Patient SafetyNet Lite Edition, clinicians can realize the benefits of Masimo's supplemental monitoring platform without a dedicated physical or virtual server, optimized for smaller institutions and individual departments. Contact your Masimo representative to discuss which Patient SafetyNet solution is right for you.
Case Study: Improving Outcomes and Reducing Costs on the General Floor
Continuous pulse oximetry monitoring in med-surg units, coupled with supplemental monitoring, may help detect patient deterioration sooner and can reduce the cost of care—as multiple studies at Dartmouth-Hitchcock Medical Center (New Hampshire), published across a fifteen-year span, have shown.
After deploying Masimo SET® with Patient SafetyNet supplemental monitoring—first in a single unit and then expanding to ~200 med-surg beds—Dartmouth-Hitchcock had zero preventable deaths due to opioid-induced respiratory depression,3 reduced unplanned ICU transfers by 50%, and reduced rescue events by 60%.4 Retrospective financial analysis showed that such reductions yielded significant operating margin improvements.5
0
Preventable deaths or brain damage due to opioid-induced respiratory depression in monitored patients over 10 years3
 50%
50%
Reduction in unplanned ICU transfers, sustained over time4
 60%
60%
Reduction in rapid response team activations, sustained over time4
$160K
Estimated Annual Savings5
$409K
Estimated Annual Savings5
For each 10% reduction in rescue events and transfer events, respectively, at a hospital with ~200 general floor beds5

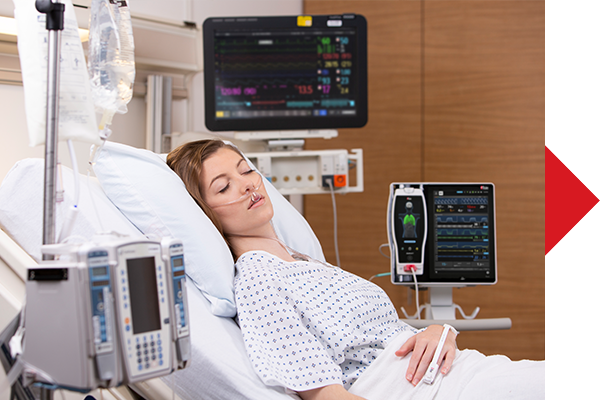
Hospital Story: Continuous Patient Monitoring in the General Care Setting
Dr. Susan McGrath, PhD, Director of Patient Surveillance Research & Development at Dartmouth-Hitchcock Medical Center, discusses how continuous monitoring—with Masimo SET® pulse oximetry on tetherless Radius PPG® sensors and Patient SafetyNet—has not only improved patient outcomes but is also improving her institution's operating margins.
As Dr. McGrath notes, "You can save patient lives, and keep them safe, using continuous monitoring—and having that system and monitoring all patients, all the time, actually can save a hospital money."
Patient SafetyNet Products & Solutions
Explore additional solutions in the Masimo Patient SafetyNet product ecosystem.
Root®
Patient Monitoring and Connectivity Hub
Expandable, customizable patient monitoring and connectivity platform

Iris® Gateway
Interoperability Solution
Automate data transfer from bedside devices into electronic medical records

Replica®
Mobile Application
View patient data from a mobile device, regardless of location
Resources
Materials
Videos
Schedule a Demo
Contact your Masimo representative or complete the form below.
Balshi AN et al. PLOS ONE. 2022;17(11):e0277992. doi:10.1371/journal.pone.0277992
The Value of Medical Device Interoperability. West Health Institute. 2013.
McGrath S et al. J Patient Saf. 2021; 17(8):557-561.
McGrath S et al. Jt Comm J Qual Patient Saf. 2016; 42(7):293-302.
Blike GT et al. J Patient Saf. 2025. 21(8():e169-175.
Caution: Federal (USA) law restricts this device to sale by or on the order of a physician. See instructions for use for full prescribing information, including indications, contraindications, warnings, and precautions.
PLCO-007908/PLM-15363A-1125 EN-PLM-11210D